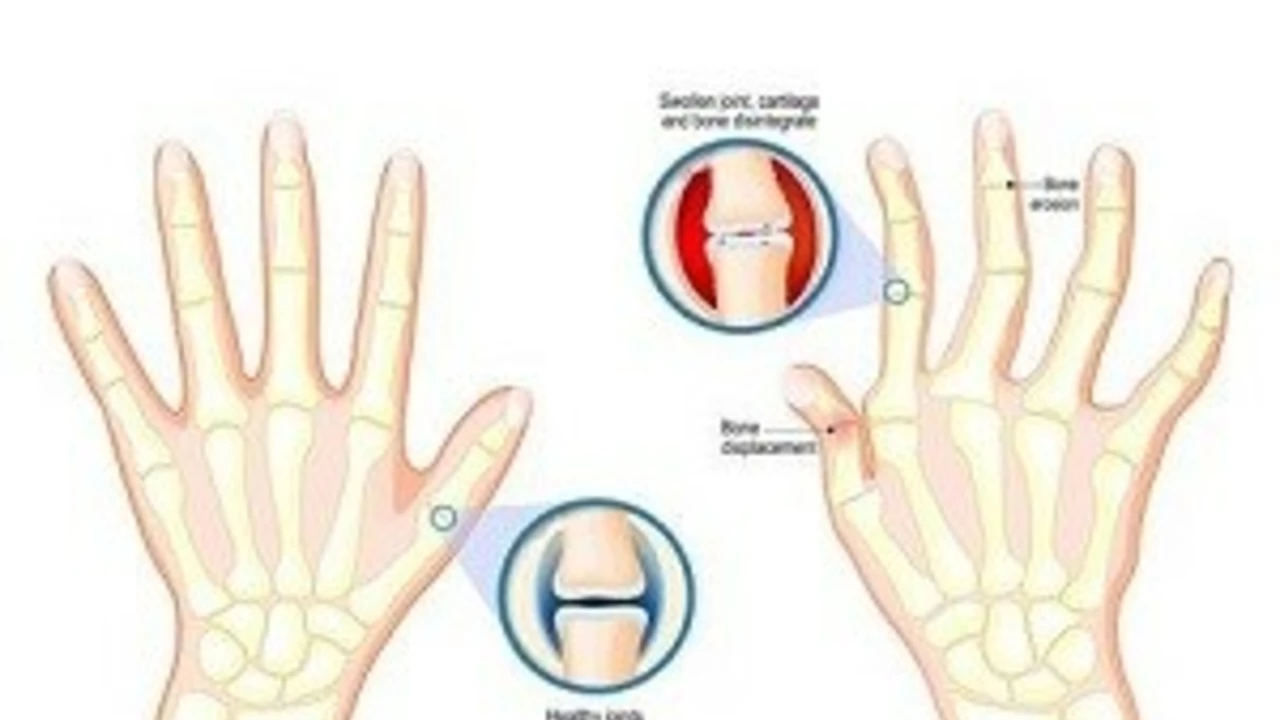
Rheumatoid arthritis: clear, practical steps to feel better
If joint pain and morning stiffness stick around for weeks, rheumatoid arthritis (RA) might be the cause. RA is an autoimmune disease that targets the lining of joints, causing swelling, pain, and over time, joint damage. Catching it early and working with a rheumatologist changes outcomes — treatment now aims to stop damage, not just ease pain.
Treatment options — what works and why
First-line drugs are called DMARDs (disease-modifying antirheumatic drugs). Methotrexate is the most common DMARD; it slows disease activity and protects joints. Other conventional options include hydroxychloroquine, sulfasalazine, and leflunomide. These need regular blood tests to watch the liver and blood counts.
If disease control is poor on DMARDs alone, doctors add biologics or targeted synthetic drugs. Biologics target immune signals like TNF (examples: etanercept, adalimumab). JAK inhibitors (tofacitinib, baricitinib) are oral options that work differently. Biologics and JAK inhibitors lower inflammation strongly but raise infection risk, so doctors review vaccines and screen for TB before starting them.
For short-term relief during flares, corticosteroids reduce inflammation fast, but they’re not a long-term solution because of side effects. NSAIDs (ibuprofen, naproxen, and COX-2 options like etoricoxib/Arcoxia) help with pain and swelling but don’t stop joint damage. Over-the-counter acetaminophen can help with pain but won’t reduce inflammation.
Daily management and when to call your doctor
Physical therapy and regular low-impact exercise (walking, swimming) keep joints mobile and muscles strong. Use heat for stiffness and cold packs for swelling. Simple joint-protection techniques — using larger joints to carry weight, using jar openers, or switching grip — make everyday tasks easier.
Watch for warning signs: sudden high fever, new shortness of breath, severe pain that limits walking, or rapid swelling. These need quick medical attention. Also report recurrent infections or unusual bruising if you’re on immunosuppressive meds.
Smoking makes RA worse and can reduce drug effectiveness. If you smoke, ask your care team for support to quit. If you’re planning pregnancy, discuss medication changes ahead of time — some RA drugs must stop before conception.
On this site you’ll find deeper articles about pain options and medication safety: guides on NSAIDs like Arcoxia, alternatives to diclofenac, long-term acetaminophen use, and natural options like willow bark or DMSO. Read those to compare risks and benefits, then bring questions to your doctor.
Practical steps right now: get a rheumatology referral if symptoms persist, track which joints hurt and when, list current meds and supplements, and ask about baseline blood tests and vaccines. Early action gives the best shot at keeping joints working and life moving.